I joined Kaiser Permanente to redesign the member-facing medical claims experience across web and mobile, with a focus on making billing information comprehensible to patients navigating complex insurance coverage.
Visa Digital Benefits Platform (VDBP) is an internal enterprise tool used by issuing banks and Visa administrators to configure cardholder benefits and packages at scale. When I joined the project, the system had a foundational problem: no organizational structure. Every variation of a benefit—different region, different card tier, different coverage limit—required creating an entirely new benefit record from scratch. Over time, the benefits library had become an unnavigable pile. Teams at issuing banks like Bradesco were slowing down, making errors, and losing confidence in the system.
Kaiser had the data. The problem was that it wasn't being surfaced in ways patients could understand. Members receiving bills after a hospital visit had no reliable way to understand what they were being charged, why the number was what it was, or what to do next. The result was predictable: confusion, anxiety, and a high volume of support calls from people who weren't disputing their bills — they just didn't understand them.
Medical billing is one of the most anxiety-producing experiences in American life. The language is opaque, the numbers are large, and the stakes are personal. Most insured members have a reasonable assumption: if they have insurance, it pays for their care. Deductibles, plan phases, copays, coinsurance — these are concepts that feel like fine print until a bill arrives.
A well-designed claims experience doesn't just reduce support calls. It reduces fear. It gives people agency over something that otherwise feels completely out of their control.
Research involved listening sessions on member support calls and review of claims-related call volume data. What emerged was a clear and consistent pattern: the gap between members who understood their claims and those who didn't wasn't about education level or financial sophistication. It was about whether the interface had ever explained anything to them.
Members who understood insurance — who knew what a deductible was, what a plan phase meant, what copay versus coinsurance meant — navigated the existing experience adequately. Everyone else was lost. And the existing design made no attempt to bridge that gap. It surfaced transaction codes, remark descriptions, and clinical terminology without translation.
One member calling in had just lost a family member and couldn't understand why she owed anything on his final claim as the account holder. The system gave her numbers. It gave her nothing else.
That research anchored every design decision that followed. The question wasn't "how do we display claim data?" It was "how do we help someone understand what happened to them financially after a medical visit?"
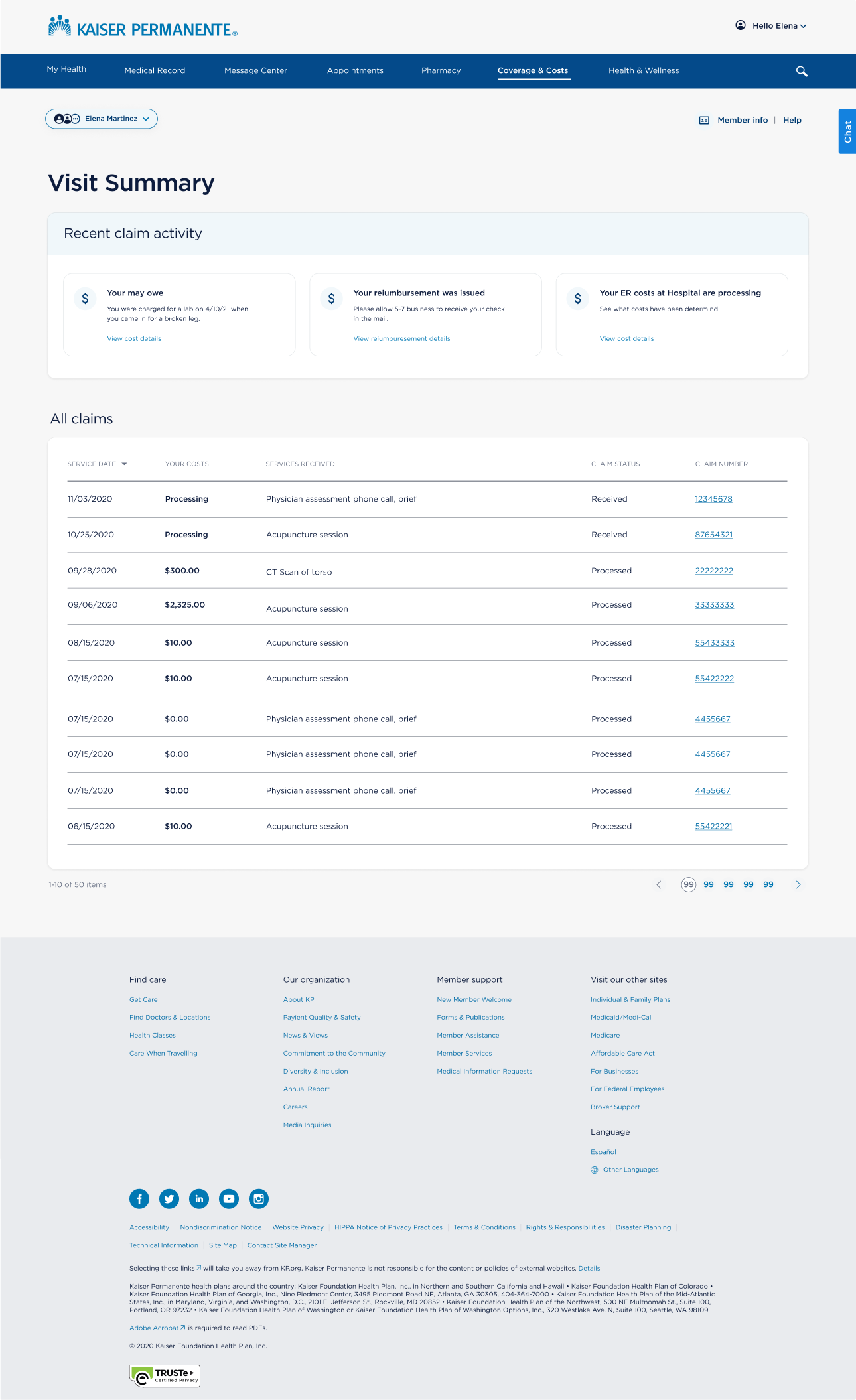
The prior claims interface showed members a table of line items — procedure codes, charge amounts, and remark descriptions — with no plain-language interpretation. Codes like "[24] Pmt adjusted, charges covered under capitation agreement / managed care plan" appeared without explanation. Members saw numbers but not meaning. The experience assumed insurance literacy that most members didn't have and didn't need to have.
The redesigned claims list surfaces the information members need before they click anything: service date, what care was received, status, and what they owe. Status badges — Pending, Paid/Approved, Denied, Reimbursement Received — are visually distinct and placed consistently so members can scan the list and understand the state of each claim at a glance.
The two most common actions — paying a bill and viewing details — are available directly on each card. Members don't have to navigate into a detail view just to find a pay button. For denied claims and claims with balances due, "View and pay bill" is the primary CTA. For claims with no balance, it's absent. The list responds to context.
Rather than navigating members away to a full detail page, the design surfaces claim detail in an overlay — accessible directly from the list without losing context. At this level, the overlay shows the services included in the claim, each with the member's share clearly labeled, and the ability to expand any line item for a full cost breakdown.
At the bottom of every claim detail, two anchors provide the essential framing: a deductible progress bar showing exactly where the member stands relative to their limit, and a "Kaiser saved you $X" callout that puts their cost responsibility in context of the total charge.
Reframing cost as savings rather than debt was a deliberate tone decision. A member who understands that their $300 bill represents Kaiser absorbing $700 on their behalf has a fundamentally different relationship with that bill. The design makes that visible — every time, for every claim.
Expanding a line item reveals the complete cost breakdown: total charge, plan rate, paid by Kaiser, paid by other insurance, copay/coinsurance, and what was applied to the deductible. The math is shown, not hidden. Members can see exactly where their bill came from without making a phone call.
The expanded view also surfaces the three-phase plan tracker: Phase 1 (You Pay Most), Phase 2 (We Share Costs), Phase 3 (No Cost), with the member's current phase highlighted and a plain-language explanation beneath. "You are in Phase 1 of your plan. You will pay full cost for most medical services." That sentence alone answers the question that was driving a significant percentage of support calls — not because members were disputing anything, but because the previous experience had never told them why.
The deductible progress bar and Kaiser saved callout persist at the bottom — so no matter how deep a member drills into their claim, the essential framing is always present.
Usability testing was conducted with actual Kaiser members across a range of insurance literacy levels. Results showed measurably improved comprehension over the existing claims experience. Members understood what they owed, why, and what to do next at significantly higher rates than with the prior design. The gap between high-literacy and low-literacy members narrowed substantially — which was the goal. The design was not doing its job if it only worked for members who already understood insurance.
This project reinforced something I carry into every healthcare and enterprise design engagement: the interface is not neutral. A claims screen that shows accurate data but explains nothing is not a neutral experience — it is an experience that works for some users and fails others along predictable lines. Designing for comprehension, not just accuracy, is an ethical position as much as a design one.
The work also sharpened my instinct for emotional context in functional design. A billing interface is not just a transaction tool. It arrives in people's lives during moments of physical vulnerability and financial stress. The "Kaiser saved you" callout, the plain-language phase explanation, the deductible progress bar — these are not decorative. They are the design doing its most important work.